The treatment of choice for symptomatic AT is catheter ablation. If these drugs are unsuccessful Class IC in combination with AV-nodal-blocking agents or Class III drugs can be tried. However not all AT are sensitive to medication and success rate of medication is usually low. Recurrent episodes of AT can be prevented with anti-arrhythmic medication, for instance with beta-blockers or calcium antagonists. If AT persist and is drug-resistant DC cardioversion can be indicated. Vagal manoeuvres or adenosine can be effective in terminating focal AT. However sometimes only an electrophysiological study can differentiate between the different SVT and localize the precise location or circuit of the AT. 
Some ATs are sensitive to adenosine and will terminate after administration of adenosine. Vagal manoeuvres or administration of adenosine can block the AV-conduction and reveal firing from the atrium, thereby clearly identifying the atrial source of the tachycardia. An ECG in resting condition of sinus rhythm can help distinguish different morphologies and help in localization of the source of the atrial tachycardia. The P-wave has a different morphology depending on the foci of the atrial tachycardia ( Figure 2). On the ECG an atrial tachycardia can be detected through the P-wave morphology. Digoxine intoxication is a common cause for ATs. Focal AT that with a progressive increase at onset and decrease before termination are likely based on abnormal automaticity. 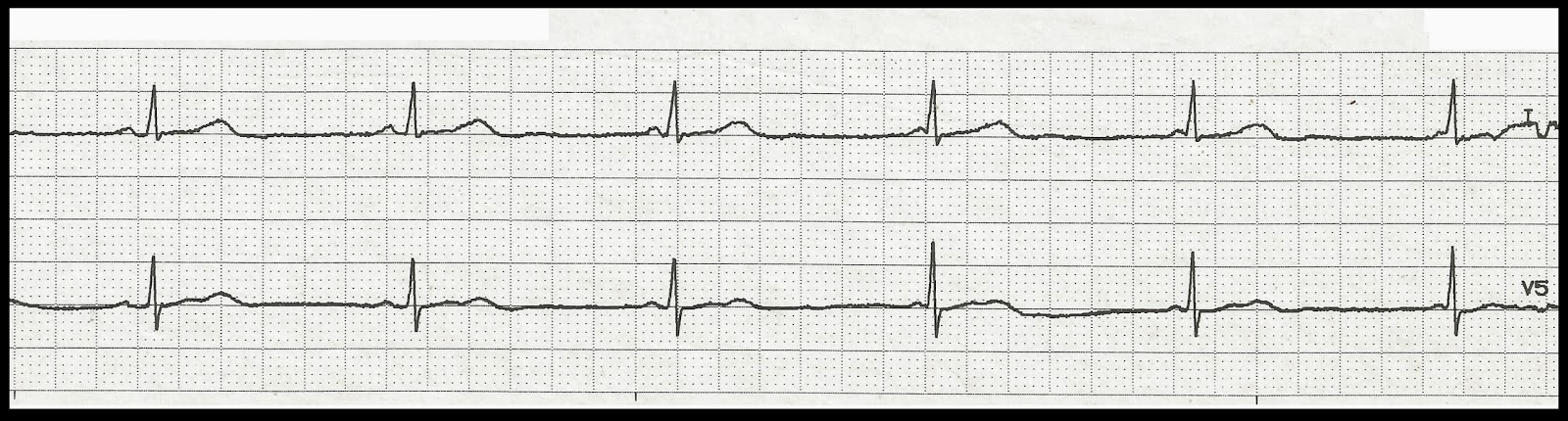
Complaints of palpitation and a fast regular heart rate are common and as a result of the tachycardia complaints of dizziness, dyspnoea and syncope can be experienced. They can occur in paroxysms or can be the permanent underlying rhythm. Atrial flutter is a distinct type of AT, but due to its unique mechanism it is discussed separately.ĪTs have a wide range clinical presentation. Patients after earlier surgery or catheter ablation usually present with macro re-entry AT located around functional or anatomical sides of block. Atrial tachycardia can be caused by all the mechanisms of arrhythmia formation. This results in different P-wave morphologies on the ECG during the arrhythmia. In some patients the tachycardia has multiple foci (multifocal atrial tachycardia). Patients with a contra-indication for beta-blockers can use nondihydropyridine calcium-channel blockers.Ītrial tachycardia (AT) is a tachycardia resulting from fast firing in an ectopic focus or micro re-entry circuit in the atria. If patients have persistent complaints, the trigger cannot be removed or in case of an inappropriate sinus tachycardia a beta-blocker can be administered. No treatment is indicated usually the sinustachycardia will pass when the external trigger is removed. An inappropriate sinus tachycardia is diagnosed by when the sinus tachycardia is persistent (therefore non-paroxysmal) and no trigger can be identified. The P-wave has the same morphology during sinus tachycardia as during normal sinus rhythm ( Figure 2). Diagnosis on the ECG can be made by the morphology of the P-wave. The term inappropriate sinus tachycardia is a persistent increase in resting heart rate or sinus rate unrelated to or an exaggerated response to stress in a person without structural heart disease.Ī sinus tachycardia usually has a gradual start and ending. External factors can increase the heart rate like coffee and alcohol or drugs. Usually it is a physiological reaction to stress (exercise, inflammation, stress). The maximum heart rate a person can achieve during exercise can be calculatedbe estimated by subtracting the age in years from 210, although it is not uncommon for sinus rates to peak above 200/min during vigorous exercise. When the sinus node fires with a frequency rate between 100-180bpm, the term sinustachycardia is used. Dependent on the refractory period of the AV-node the ventricles follow the atrial activation at the same rate at higher atrial rates the AV-node starts to block conduction from atrium to ventricle. The following arrhythmias arise in the atrium. Supra-ventricular tachycardia Atrial arrhythmias VTs can both take place in the myocardial tissue and the conduction system tissue ( Figure 1). VT's are rhythm disorders that origin from the ventricles. Supraventricular arrhythmias are relatively common and rarely life-threatening. SVT's are arrhythmias in the atria or AV-node or arrhythmias in which these structures are involved. Classification of tachyarrhythmias.ĭifferentiation between supraventricular tachycardias (SVT) and ventricular tachycardias (VT) can be challenging, especially in acute emergency settings.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
